What is Carrier Screening?
Genetic carrier screening is for everyone. It is a way to determine whether an individual is a carrier of a genetic mutation that may be passed along to a child. Studies have shown that most people carry at least one disease-causing change, also known as a “mutation.” Some of these changes may cause a serious, possibly fatal, condition in a child. Carrier screening – best done before pregnancy – can identify carrier parents and enable them to build healthy families.
Carriers
Our genes come in pairs, one from each parent. A carrier of an autosomal recessive disease is an individual who has a mutation in one copy of a particular gene that causes the gene not to function properly. Since carriers have a second working copy of the gene, they generally do not develop any symptoms of the disease, but they can pass on the gene with a mutation to their children.
Recessive Genetic Diseases
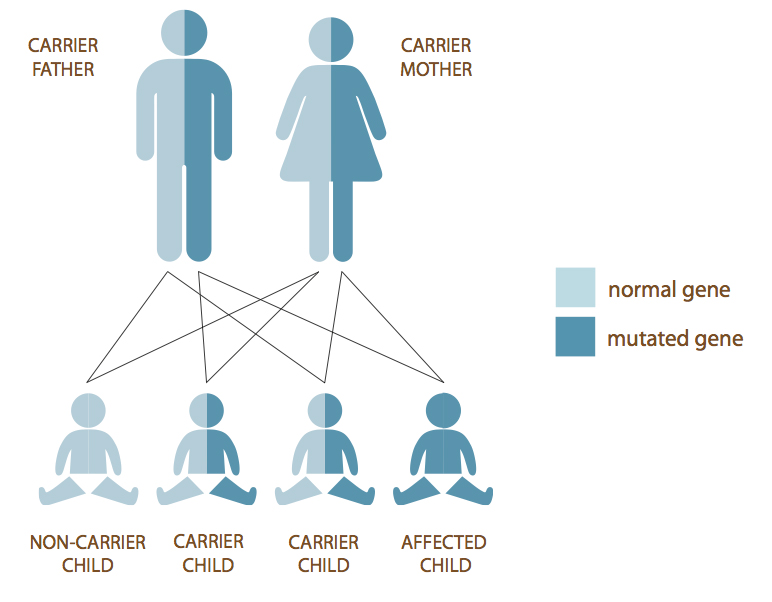
Autosomal recessive diseases are those that develop when both parents are carriers of the same condition and they both pass on their mutations to their child. Many diseases that are common in the Jewish population are inherited in an autosomal recessive pattern.
Special Circumstances
While carrier screening generally identifies carriers of recessive diseases, some individuals may discover, during the course of carrier screening, that they themselves have two mutations and are at-risk for one of the less severe or late-onset diseases on the testing panel. It is important that results be discussed with a genetic counselor.
What screening should be done?
Expanded carrier screening should be done for anyone planning to start or add to their family, preferably before any pregnancy.
Ancestry and other genetic testing
While testing for ancestry and predisposition to certain diseases does involve genetic testing, carrier screening for recessive diseases is not the same. It is important that you speak with someone knowledgeable in genetics to learn the difference and become aware of what kind of information you may learn from any form of genetic testing before proceeding. You may learn a lot about family and your own health risks that you did not expect.
Cancer Genetic Testing
You may have heard that Ashkenazi Jews are more likely than others to have mutations in the BRCA gene, which could predispose carriers to certain cancers. Reproductive carrier screening will not tell you if you carry BRCA or any other hereditary cancer mutation. If you have a personal or family history of cancer, or if you would like to know if you carry a mutation and are at risk of developing cancer, a consultation with a genetic counselor is recommended
Who should be screened?
Screening is for everyone
Everyone considering having children should be screened. While many diseases are more commonly found in certain ethnic groups, there is still a chance that an individual from a different background might be a carrier, as well.
Screening a couple
At least one member of every couple should be screened. If his or her results are positive, the other member of the couple should then be screened. Some couples decide to be screened simultaneously, as to avoid the waiting between results especially if they are already pregnant.
Female specific screening
There may be some diseases on the testing panel for which only females are screened. Therefore, if one partner is tested first, it is recommended that the female be first.
How is screening done?
Screening using blood or saliva
Carrier screening for all of the Jewish genetic diseases by DNA analysis can be done using blood or saliva. For Tay-Sachs disease screening, enzyme analysis using blood is optional, as new research has established that comprehensive DNA sequencing of the Tay-Sachs gene is just as accurate as enzyme analysis.
Reviewing results
All genetic tests should be ordered and the results read by a knowledgeable physician or genetic counselor trained to interpret such results. Pre-test education and post-test counseling are recommended with any form of genetic testing. Please be aware that not all genetic testing companies provide these services.
Updating screening
Diseases are often added to panels, so be sure testing is up-to-date before any pregnancy. Individuals should always request a copy of their results, which should be kept it in a safe location.
Cost and insurance coverage
Cost and insurance coverage depend on which lab or genetics program you are using. Some have set out-of-pocket prices and may bill your insurance, some provide free testing at on-site events, and others will bill your insurance and charge you the balance. Medical genetics programs can be helpful in determining coverage. Please note that some labs offer financial assistance programs for eligible individuals.
Financial assistance
The JGDC may be able to help identify resources for carrier screening for those who do not have insurance or need assistance with coverage. Please contact the JGDC at info@jewishgeneticdiseases.org for more information.
Where is carrier screening done?
Currently there are several places to obtain screening: a hospital or clinic-based medical genetics program, an online genetics program that offers education, counseling and screening, or your physician’s office.
When is the best time to be screened?
Screening before pregnancy
Screening before pregnancy is optimal. This allows carrier couples the greatest number of reproductive options. Diseases are often added to testing panels, so be sure testing is up-to-date before any pregnancy.
What are options for carrier couples?
Know your options
There are multiple reproductive options that enable carrier couples to build a healthy family. Each couple needs to make their own informed decision, based on the disease or diseases for which they are carriers, and other personal considerations. Genetic counselors can explain options in depth.
During pregnancy
A carrier couple may choose to become pregnant and test the fetus early in the pregnancy, either by chorionic villus sampling (CVS) or amniocentesis. In the case of an affected fetus, the couple can decide how to proceed with the pregnancy. In order to test the fetus, the parents’ carrier statuses must be known
Before pregnancy
A carrier couple may choose…
- To undergo In-vitro fertilization (IVF) with pre-implantation genetic testing (PGT). In this procedure, the egg is fertilized outside the body and embryos are tested at a very early stage for the disease(s) carried by the parents. Only unaffected embryos are implanted in the womb.
- To use egg or sperm from a screened non-carrier donor
- To adopt
- Not to have children
- Not to continue the relationship